Generalized periodontitis: symptoms and treatment
Periodontitis is a very common pathology of periodontal tissues (soft tissue structures around the dental unit). If the pathological process is started and left without treatment, then you can lose all the dental units.
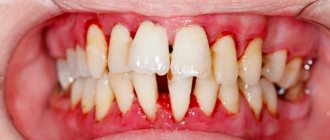
Periodontal pockets are the best location for the emergence and development of an infectious process, which does not have the best effect on the healthy state of the body. A beautiful and healthy smile gives you self-confidence and makes you feel natural. When periodontal tissue is damaged, the gums become red and swollen. The disease affects the overall health of the body and the well-being of a person. If something bothers you in the oral cavity, you should immediately consult a specialist. Dentist therapists at the branches of the West Dental family clinic in Yanino-1 and Vsevolozhsk will help with identifying the origins of anxiety and their treatment.
It has been scientifically determined that the occurrence of periodontitis is influenced by: soft plaque and hard deposits; filling material or orthopedic structure fixed in violation of treatment protocols.
Advantages of treatment at JSC "Medicine"
By contacting JSC “Medicine” (clinic of Academician Roitberg), you can be sure that the examination will be carried out as completely as possible and exclusively using high-precision equipment. From the first contact to receiving test results, no more than a day passes. Also, each patient of the clinic is provided with:
- an accompanying person to move around the clinic;
- personal physician-supervisor who will monitor the progress of diagnostics and treatment processes;
- written recommendations regarding treatment and all necessary information regarding prescribed medications.
At the clinic of JSC "Medicine" you will not waste your personal time in line. Our medical center provides services at an international level of quality, and if controversial issues arise, the administration is always ready to consider any requests.
Classification
According to the number of units affected by pathology:
- Catarrhal (localized) – 1-3 units in the affected area;
- Generalized – the entire dentition is affected.
According to the severity of generalized periodontitis (ICD code K05):
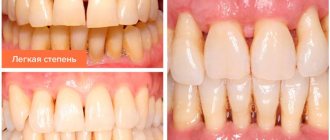
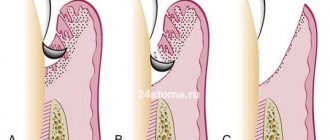
- Generalized mild periodontitis (ICD 10 code K05.3). This clinical diagnosis is made when the depth of the pockets in the gingival tissue is less than 3.5 mm, and less than 1/3 of the root is resorbed.
- Average. The subgingival depressions are 3.5-5 mm, and the bone is sclerosed at 50% of the root length.
- Severe degree. This stage is indicated by the depth of periodontal changes greater than 5 mm and resorption of more than 1/2 of the root.
Differential diagnosis according to pathogenesis:
- acute - more than one annual exacerbation;
- chronic generalized periodontitis (according to ICD K05) is an ongoing pathological process;
- exacerbation of chronic periodontitis – pain, discomfort, activation of the inflammatory process.
Indications
Vitamins A and C are especially important for patients with periodontitis. It is necessary to include more fruits, vegetables and herbs in the diet. At an early stage, when the teeth are not yet loosened, you can eat the fruits in solid form. This will ensure the necessary load on the dental system. It is necessary to chew on both sides, and not just one, so that all areas of the teeth work actively. It is useful to include the following products in the menu:
- seafood;
- apples;
- Bell pepper;
- avocado;
- dill, parsley;
- black currant berries;
- carrot;
- peanut;
- citrus.
The diet must include dairy products, which are a source of calcium. The patient needs to consume more milk, sour cream, cottage cheese, and different types of cheese. Vitamin A, which promotes epithelial regeneration, is found in pork and beef liver, pumpkin, apricots, broccoli and spinach. Zinc, which is present in lentils, peas, and seafood, is useful for bone tissue. If you have periodontal disease, it is better to drink green tea or natural juices.
Symptoms
The initial symptoms of the inflammatory process in periodontal tissues are the following:
- swelling of the gum tissue;
- severe bleeding during and after cleaning;
- throbbing severe pain.
As the pathology spreads, symptoms intensify:
- enlarged and painful lymph nodes;
- unpleasant odor from the mouth;
- mobility of dental units;
- increased sensitivity of tooth enamel;
- pain when biting and chewing food;
- deterioration of the general condition of the body;
- purulent discharge from periodontal pockets.
Chronic generalized periodontitis (beyond exacerbation) is characterized by:
- reddish color of gum tissue;
- exposure of tooth roots;
- Bone resorption is visually determined on the Rg image.
Chronic generalized periodontitis
Chronic generalized periodontitis (according to ICD 10-K05) affects the soft tissue and bone structures of all or more dental units. The frequency of occurrence is 5 times higher than carious lesions and its possible complications. Also, a generalized process can most likely lead to complete edentia (lack of teeth). The long-term location of the infectious process in periodontal tissues, without proper treatment, negatively affects the body's immune defense and can contribute to the development of rheumatoid arthritis, heart disease, etc. Generalized periodontitis has a different etiology.
Diagnostics
To determine the disease and its severity, various diagnostic methods are used. For generalized periodontitis, differential diagnosis includes an extensive consultation examination to draw up a medical history (formation plan):
- collection of complaints (mobility of units, discomfort when chewing, periodic sharp pain in the attached gum);
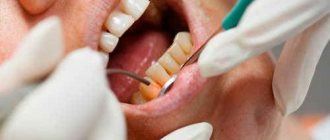
- visual and instrumental examination (gingival pockets, recession of gingival tissue, dental plaque, reddish gums);
- determination of the color, shape and structure of gum tissue;
- finding out what condition the dental units are in: percussion, palpation, degree of mobility;
- determination of hygiene indices;
- RG images.
Sometimes, a specialist may prescribe a blood test to clarify the etiology.
Diagnostic measures should take into account not only all the symptoms of the pathology and the patient’s complaints, but also the mandatory performance of an X-ray. Basically, in case of periodontitis, it is recommended to perform an OPTG (orthopantomogram) - a panoramic image. In such an extensive image, all dental structures and the degree of bone damage in each unit are immediately visible.
Mild degree
As usual, mild degrees are not given any importance. A subgingival pocket is formed near the dental unit, where microorganisms accumulate. There are signs of periodontal inflammation, and on the Rg image there is destruction of bone tissue by 1/3 of the root, gum pockets up to 3.5 mm. In the cervical area of the teeth, hard deposits are observed, the gums are loose, slightly inflamed and swollen. There is slight bleeding when cleaning, and discomfort when chewing solid food. Mobility and movement of teeth is not observed at this stage.
Degree of tooth mobility
With periodontitis, teeth gradually become loose. Depending on their mobility, there are 4 degrees of the disease:
- 1st degree, when the tooth moves no more than 1 mm to the adjacent tooth, in the bucco-lingual and vestibulo-oral directions;
- 2 degree, in which mobility is observed in the same directions as in the first degree, but only by more than 1 mm;
- 3rd degree. Teeth become mobile in any direction, including vertical;
- 4th degree. Mobility is observed in all directions, and the tooth can even rotate around its axis.
Average degree
With moderate severity, periodontal pockets up to 5 mm are observed. The x-ray shows damage to the bone septa on half the root. In the oral cavity, upon examination, there is a sufficient number of dental deposits, mobility of teeth I-II degrees, inflammation of the gums. A small amount of pus may ooze from under the gums. When the process worsens, slight mobility and displacement of units occurs.
Patients complain of pain in the gums; pain and bleeding when eating; the necks of the teeth are exposed; a reaction to cold and hot food is formed.
Severe degree
Chronic generalized severe periodontitis, as diagnosed, is determined by deep periodontal pockets over 5 mm and 2/3 of the tooth root being exposed. With this degree of pathology, great swelling, bleeding and hyperemia of the gums occurs, and eating is quite painful. In periodontal pockets there is a large accumulation of pus and microorganisms in the form of dental deposits. Patients have complaints of pain, itching, burning and pulsation in the gums. It is impossible to carry out high-quality hygienic cleaning on your own; a persistent unpleasant odor persists for a long time. In the absence of proper therapy, severe suppuration and mobility of grade III-IV units are observed, up to prolapse. Complications may develop in the form of abscess formation of foci of infection and periodontal disease.
Also, this pathology is manifested by a violation of the general condition of the body. A person is worried about weakness, fever, and in connection with this, fatigue. Regional submandibular lymph nodes enlarge and become painful on palpation.
Surgical intervention
When the depth of the periodontal pocket exceeds 5 mm, doctors decide on surgical treatment. In this case, a flap operation is performed - gingivectomy. It is carried out according to the following scheme:
- The gum is dissected, after which the gum flap in the area of the periodontal pocket is turned away.
- Next, the tooth root is cleaned and destroyed tissues and microorganisms are removed from the pocket.
- Then the tissues are washed with an antiseptic, after which the gum flap is returned to its place and sutures are applied.
The duration of the operation can be from 1 to 3 hours, it is performed under local anesthesia. During the process, the doctor can also straighten the bone tissue if inflammation has already spread to it. Depending on the nature of tissue damage, other operations may be performed:
- Gingivoplasty is a soft tissue transplantation. It is carried out when they are completely atrophied, when the tooth is completely exposed and visually becomes longer. To cover the defects, tissues from the palate are used. This helps stop the deepening of the periodontal pocket.
- Osteoplasty. It is carried out in case of destruction of bone tissue by inflammation, which can no longer hold the tooth in its place. During the operation, a graft made of bone tissue or synthetic material is used.
Another surgical method for treating periodontitis is splinting mobile teeth. This procedure allows you to keep them in place and save them from spontaneous removal. Splinting today is carried out in different ways:
- A horizontal bar and fiberglass tape are placed over several teeth. Then everything is filled with a light composite, as a result of which the dentition is connected.
- On the teeth, the upper part of which is previously ground down, crowns are put on, welded together.
- A clasp prosthesis is placed on the jaw, which allows you to evenly distribute the load on both the teeth and gums, and when installed on the upper row, on the upper palate.
Treatment
When the pathological process has taken the form of chronic generalized periodontitis, it is more difficult to carry out effective treatment. It is important to address the underlying cause of the disease. In this regard, the generalized form of periodontitis requires consultation with dentists in related fields to identify the source of the pathology. The general dentist/periodontist can provide recommendations for consultation with an endocrinologist, hematologist, immunologist, etc. After general interaction and identification of the cause of periodontitis, the attending physician prescribes the necessary therapy.
Treatment of the pathological process consists of the following measures:
- Professional oral cleaning and hygiene training. A specialist removes soft and hard dental deposits, including those under the gums. The tooth enamel is polished with special brushes with paste and coated with a protective gel with fluoride. Oral care products are selected and instructions on their use are provided.
- Treatment of associated dental problems. To cure periodontitis, it is important to treat caries, pulp disease, and pathological processes in the gums and bones.
- Drug therapy. Oral baths with solutions, application ointments, NSAIDs and painkillers, and sometimes antimicrobial drugs are used.
- Removal of subgingival pockets by a dental surgeon. In case of moderate and severe severity, it is possible to perform open and closed curettage of pockets, as well as gum plastic surgery.
- Treatment using orthopedic structures. As part of complex measures, temporary splinting of mobile units is performed with an orthodontic retainer or fiberglass; selective grinding of the chewing surfaces of teeth; prosthetics of large dental defects to redistribute chewing pressure.
- Physiotherapeutic manipulations. Many physiotherapy procedures have a positive effect on recovery: UHF, infrared radiation, magnet and laser therapy, electrophoresis, direct and alternating current, vacuum and acupressure massage, paraffin therapy, mud therapy.
For effective treatment of pathology and the occurrence of remission of the process, it is important to fully comply with the specialist’s instructions.
Why you can’t install removable and bridge dentures against the background of advanced periodontitis
Loss of bone tissue and widening of the sockets during periodontitis create a very ambiguous situation: on the one hand, long-term conservative treatment in the later stages is rarely effective, on the other hand, prosthetics are also difficult, and the problem of missing teeth needs to be solved. However, not every treatment method is suitable.
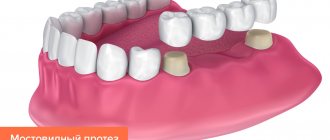
Why are dental bridges not suitable?
Teeth with periodontitis are weakened and are on the verge of falling out; it is strictly forbidden to use them as support for a denture. The bridge will be movable along with the teeth on which it is attached. The risks are high, even if complex and long-term treatment was carried out before.
Why are removable dentures not suitable?
In fact, after a course of treatment for periodontitis (or closer to the middle of it after acute inflammation has resolved), removable dentures can be installed to solve the problem of partial absence of teeth. But only for a short time, because... When used long-term, they lead to many problems:
- do not stop bone atrophy, but only aggravate this process,
- put increased pressure on the gums and can provoke inflammation, which is extremely undesirable during the course of therapy,
- will require regular correction, since during treatment the damaged tissues are restored, which means the level of the bone with the gum will change - the dentures will no longer fit tightly, will shift, dangle,
- if teeth are partially missing, there is nothing to attach them to - as in the case of bridges, it is better not to use living teeth for support, especially if they are mobile,
- if the teeth are removed scatteredly, then removable dentures will not work at all; the minimum segment is 2-3 missing teeth in a row.
That is, removable dentures can provoke the development of periodontitis and negate all the results of a course of complex treatment. In addition, they are difficult to get used to - more than half of patients are not satisfied with them either in aesthetics or functionality.