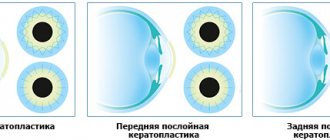
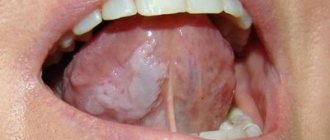
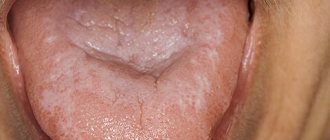
The development of dental pathologies, as a rule, is a consequence of the progression of pathological processes occurring inside the human body. Against the background of weakened immunity, the influence of external negative factors increases, which leads to the formation of problem areas. The causes of diseases can be different: by the symptoms manifested on the tongue, lips and gums, as well as by the results of clinical diagnostics, including the use of professional equipment, the source of concern can be determined. Classification of diseases of the oral mucosa helps to make a correct diagnosis and begin therapy in a timely manner, avoiding more serious negative consequences.
Classification of diseases of the oral mucosa
Stomatitis
Stomatitis is an inflammation of the mucous membrane, characteristic of children and adults. Most often, stomatitis is bacterial, viral or fungal in nature. A bad toothbrush with hard, scratchy bristles, poorly fitting braces or crowns, and biting the cheeks and lips can also cause canker sores.
Most often, stomatitis manifests itself in the form of itchy, bright red or whitish sores and erosions on the inner surface of the cheek, tongue or gums. A person may complain of burning and swelling, bad breath, pain when chewing and swallowing. In advanced cases, the temperature may rise, sleep may be disturbed, and the person becomes irritable.
Glossitis
Glossitis is an inflammation of the tongue that can occur either as a result of injury (such as a burn), exposure to pathogens, or as a symptom of certain systemic diseases. Most often, glossitis is manifested by a burning sensation and discomfort in the mouth. The tongue becomes bright red and slightly swollen, and salivation may increase. The patient may complain of loss of taste or changes in the sense of taste, and eating or even just talking causes pain.
Highlit
Haylit (or cheilosis) is a disease in which the lips begin to peel, break, and “sticks” appear in the corners of the mouth. The reasons can be very different: exposure to wind and sun, allergic reaction, chronic diseases with skin lesions (dermatitis, psoriasis, etc.), endocrine pathologies or mycoses.
Oral leukoplakia
Oral leukoplakia is keratinization of the mucous membrane under the influence of aggressive factors, such as smoking. This condition is considered precancerous and therefore requires mandatory treatment.
Most often, oral leukoplakia appears as whitish, grayish, or red plaques that cannot be removed, rough or keratinized areas, or strange thickenings on the lining of the mouth. As a rule, the patient does not experience pain or discomfort, and therefore does not immediately consult a doctor.
Paradontosis
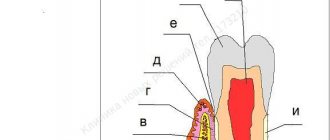
The periodontium is the complex of tissues that surround the tooth and hold it in place: the gums, periodontal ligament, periodontium, root cementum and bone tissue. Periodontal diseases include: gingivitis, periodontitis and periodontal disease.
Gingivitis
Gingivitis is an inflammation of the gums that most often occurs due to inadequate or irregular oral hygiene. Pathogens accumulate in plaque and tartar, causing inflammation.
With gingivitis, inflammation affects only the surface of the gums and may cause bleeding, swelling of the gums, mild pain or discomfort when pressing, and bad breath. If treatment is not started, the inflammation will go further and affect the periodontium.
Periodontitis and periodontal disease
Very often, patients confuse periodontitis and periodontal disease. Periodontitis is an inflammatory disease of periodontal tissues that causes bleeding gums and leads to the gradual exposure of tooth roots, their mobility and, as a result, their loss. Periodontal disease is a non-inflammatory periodontal disease in which the lining of the gums and jaw bone gradually decrease. Unlike periodontitis, in which tooth tissue is destroyed over several years, periodontal disease progresses very slowly and develops over decades. The patient may not even realize that he has gum disease. Periodontal disease is rare compared to other oral diseases.
Caries
According to a study published in the medical journal The Lancet, 2.83 billion adults and children worldwide have tooth decay.
Cavities typically form when bacteria in plaque combine with sugar to form an acid that erodes enamel.
Treatment:
If you or your dentist catches tooth decay early enough, you may be able to reverse the process with fluoride medications. Otherwise, the classical treatment of caries is provided - filling.
However, if the decay gets so bad that a filling doesn't help, your dentist may crown the tooth or remove it. Again, early detection can prevent tooth decay and loss.
Causes of development of diseases of the oral mucosa
- Traumatic damage to oral tissues and other traumatic effects (chemical, thermal, etc.) with the development of traumatic erosion, ulcers, leukoplakia or leukokeratosis (keratinization of the mucous membrane, capable of malignant degeneration).
- Infectious diseases that affect the oral mucosa due to the penetration of viruses, spirochetes, bacteria, and fungi.
Quite often, the occurrence of pathological changes in the oral mucosa is associated with disruption of various organs and systems of the body: allergies, dysfunction of the cardiovascular system, gastrointestinal tract, endocrine disorders, systemic connective tissue diseases, blood diseases and other dermatoses, tuberculosis, AIDS and some other conditions.
Brief conclusions
- The most common oral diseases are tooth decay, gum disease, infectious diseases and oral cancer.
- Caries and gum disease are highly treatable in the early stages.
- The causes of infectious diseases of the oral cavity vary - from viruses to poor diet and uncontrolled use of medications.
- For prevention, it is important to review “life hygiene” and regularly visit the dentist.
Anti-Aging Medicine Seminars Gain knowledge based on evidence-based medicine first-hand from the world's leading experts. As part of the Anti-Age Expert Modular School, in-person two-day seminars are held every month, where the intricacies of anti-age medicine are revealed to doctors of more than 25 specialties
Find out more
Diagnosis of pathologies
Modern techniques used in dentistry make it possible to quickly identify infectious or fungal diseases of the oral mucosa. It is worth noting that self-diagnosis, as well as subsequent attempts at self-medication, often cause a deterioration in the general condition. Determining the causes of pathological changes is a medical task for which the following are used:
- Microscopic examination of samples.
- Test for allergic reactions.
- Test for viral pathogens.
- General examination and medical history.
Timely diagnosis is necessary to develop and implement the correct treatment plan that addresses both negative symptoms and factors that are proven to cause pathological changes.
Principles of treatment of diseases of the oral mucosa
Basic principles of treatment of diseases of the mucous membranes of the mouth, lips and tongue:
- Rational treatment requires contact between the dentist and other dental and non-dental professionals.
- Treatment must be carried out in compliance with the principles of bioethics, these diseases must be considered from the point of view of the state of the whole organism, therefore in most cases one cannot limit oneself to local effects only.
- An axiom for the dentist should be the elimination of all unfavorable irritating factors in the patient’s oral cavity that can support and provoke the development of the pathological process. The use of so-called cauterizing agents and prolonged use of the same mouth rinses is unacceptable.
- Treatment should begin only after at least one preliminary diagnosis has been established and the following requirements have been met: be comprehensive; provide a pathogenetic approach; do not violate the anatomical and physiological characteristics of the oral mucosa; eliminate the pain factor; promote rapid epithelization of lesions; provide for the active involvement of the patient in performing treatment procedures at home.
Therapy methods
- Etiotropic and pathogenetic therapy aimed at eliminating the cause of the disease (antiviral, antibacterial therapy due to the infectious nature of stomatitis, glossitis, cheilitis, vitamin therapy for hypovitaminosis, treatment of the underlying disease that caused the appearance of a pathological process in the oral cavity) of the mucous membrane;
- Local treatment aimed at eliminating local traumatic factors, the main symptoms of the disease and faster healing of existing erosions and ulcers;
- A general strengthening procedure that stimulates the body's defenses.
NON-ODONTOGENIC AND SPECIFIC INFECTION
NECROTIC STOMATITIS (VINCINS ULCER-NECROTIC GINGIVOSTOMATITIS)
Main pathogens
Fusobacterium is concentrated in the gingival sulcus
, pigmented
Bacteroides
, anaerobic spirochetes. With necrotizing stomatitis, there is a tendency for infection to quickly spread into surrounding tissues.
The causative agents are F. nucleatum, T. vinsentii, P. melaninogenica, P. gingivalis and P. intermedia
.
In patients with AIDS, C. rectus
.
Choice of antimicrobials
Drugs of choice:
phenoxymethylpenicillin, penicillin.
Alternative drugs:
macrolide + metronidazole.
Duration of therapy:
depending on the severity of the current.
ACTINOMYCOSIS
Main pathogens
The main causative agent of actinomycosis is A.israelii
, association with gram-negative bacteria
A. actinomycetemcomitans
and
H. aphrophilus
, which are resistant to penicillin but sensitive to tetracyclines, is also possible.
Choice of antimicrobials
Drugs of choice
: penicillin at a dose of 18-24 million units/day, with positive dynamics - transition to step-down therapy (phenoxymethylpenicillin 2 g/day or amoxicillin 3-4 g/day).
Alternative drugs
: doxycycline 0.2 g/day, oral drugs - tetracycline 3 g/day, erythromycin 2 g/day.
Duration of therapy
: penicillin 3-6 weeks IV, drugs for oral administration - 6-12 months.
Prevention
To prevent painful symptoms, experts recommend following the universal rules of oral hygiene:
- use properly selected toothbrushes, use them systematically, and also avoid bad habits, especially smoking.
- It is recommended to control your diet: in some cases, oral irritation may be caused by excessive consumption of oranges, lemons, etc.
- the habit of cleaning seeds with teeth rather than with hands can become unfavorable for the oral cavity.
Literature
- Banchenko G.V. Combined diseases of the oral mucosa and internal organs. - M.: Medicine, 1979. - 190 p.
- Banchenko G.V., Maksimovsky Yu.M., Grinin V.M. Language is the “mirror” of the body: Clinical guide for doctors. - M., 2000. - 408 p.
- Borovsky E. V., Danilevsky N. F. Atlas of diseases of the oral mucosa. — 2nd ed., revised. and additional - M.: Medicine, 1991. - 320 p.
- Danilevsky N. F., Leontyev V. K., Nesin A. F., Rakhniy Zh. I. Diseases of the oral mucosa. - M., 2001. - 271 p.
- Diagnosis, treatment and prevention of dental diseases / V. I. Yakovleva, E. K. Trofimova, T. P. Davidovich, G. P. Prosveryak. — 2nd ed., revised and supplemented. - Mn.: Higher. school, 1994. - 494 p.
- Dmitrieva L. A., Glybina N. A., Glybina T. A. et al. Experimental substantiation of the use of a new antioxidant drug in the treatment of erosive and ulcerative lesions // Periodontology. — 2012, No. 3 (64). - pp. 52-58.
- Diseases of the mucous membrane of the mouth and lips / Ed. prof. E. V. Borovsky, prof. A. L. Mashkilleyson. - M.: Medicine, 1984. - 400 p.
- Diseases of the oral mucosa: Textbook / Ed. L. M. Lukinykh. - N. Novgorod: Publishing House of NGMI, 1983. - 212 p.
- Karakov K. G., Vlasova T. N., Oganyan A. V., Pisarev G. Yu. Optimization of complex therapy of lichen planus of the oral mucosa // Dentist-practitioner. - 2012, No. 1. - P. 35-37.
- Karakov K. G., Vlasova T. N., Oganyan A. V., Polyakova O. V. The role of complex therapy in the treatment of herpetic infection of the dental system // Practitioner dentist. - 2012, No. 2. - P. 48-49.
- Practical guide to anti-infective chemotherapy / Ed. L. S. Strachunsky, Yu. B. Belousov, S. N. Kozlov. - M.: Borges, 2002. - 384 p.
- Rybakov A. I., Banchenko G. V. Diseases of the oral mucosa. - M.: Medicine, 1978. - 232 p.
- Therapeutic dentistry: textbook: 3 hours / ed. G. M. Barera. - M.: GEOTAR-Media, 2055. - Part 3. - 288 p.
- Tretyakovich A. G., Borisenko L. G., Pishchinsky I. A. Differential diagnosis and principles of treatment of diseases of the oral mucosa: educational method. allowance. — 2nd ed., revised. and additional - Mn.: BSMU, 2005. - 66 p.
- Udzhukhu V. Yu., Minatulaeva M. A., Kubylinsky A. A. Pathogenetic rationale and clinical effectiveness of the use of Lavomax in patients with exudative erythema multiforme // Farmateka. - 2008, No. 9. - P. 60-62.
- Tsepov L. M., Nikolaev A. I. Medical tactics for erosive and ulcerative lesions of the mucous membrane of the mouth, tongue and lips (Training manual). - Smolensk: SGMA, 2005. - 16 p.
ODONTOGENIC AND PERIODONTAL INFECTION
PULPITIS
Main pathogens
Viridans streptococci ( S. milleri
), non-spore-forming anaerobes:
Peptococcus
spp.,
Peptostreptococcus
spp.,
Actinomyces
spp.
Choice of antimicrobials
Antimicrobial therapy is indicated only in case of insufficient effectiveness of dental procedures or spread of infection into surrounding tissues (periodontal, periosteal, etc.).
Drugs of choice
: phenoxymethylpenicillin or penicillin (depending on the severity of the disease).
Alternative drugs
: aminopenicillins (amoxicillin, ampicillin), inhibitor-protected penicillins, cefaclor, clindamycin, erythromycin + metronidazole.
Duration of use
: depending on the severity of the current (at least 5 days).
PERIODONTITIS
Main pathogens
Microflora is rarely detected in the periodontal structure and is usually S.sanguis, S.oralis, Actinomyces
spp.
In periodontitis in adults, gram-negative anaerobes and spirochetes predominate. P.gingivalis, B.forsythus, A.actinomycetemcomitans and T.denticola
are highlighted most often.
In juveniles, there is rapid involvement of bone tissue in the process, with A. actinomycetemcomitans
and
Capnocytophaga
spp.
P.gingivalis
is rarely isolated.
In patients with leukemia and neutropenia after chemotherapy along with A. actinomycetemcomitans
C.micros
is isolated , and in prepubertal age -
Fusobacterium
spp.
Choice of antimicrobials
Drugs of choice
: doxycycline; amoxicillin/clavulanate.
Alternative drugs
: spiramycin + metronidazole, cefuroxime axetil, cefaclor + metronidazole.
Duration of therapy
: 5-7 days.
For patients with leukemia or neutropenia after chemotherapy, cefoperazone/sulbactam + aminoglycosides are used; piperacillin/tazobactam or ticarcillin/clavulanate + aminoglycosides; imipenem, meropenem.
Duration of therapy
: depending on the severity of the course, but not less than 10-14 days.
PERIOSTITIS AND OSTEOMYELITIS OF THE JAWS
Main pathogens
With the development of odontogenic periostitis and osteomyelitis, S. aureus
, as well as
Streptococcus
spp., and, as a rule, anaerobic flora prevails:
P.niger, Peptostreptococcus
spp.,
Bacteroides
spp.
Specific pathogens are less commonly identified: A.israelii, T.pallidum
.
Traumatic osteomyelitis is often caused by the presence of S.aureus
, as well as
Enterobacteriaceae
spp.,
P.aeruginosa
.
Choice of antimicrobials
Drugs of choice
: oxacillin, cefazolin, inhibitor-protected penicillins.
Alternative drugs
: lincosamides, cefuroxime.
When P.aeruginosa
, antipseudomonas drugs (ceftazidime, fluoroquinolones) are used.
Duration of therapy
: at least 4 weeks.
ODONTOGENIC MAXILLARY SINUSITIS
Main pathogens
The causative agents of odontogenic maxillary sinusitis are: non-spore-forming anaerobes - Peptostreptococcus
spp.,
Bacteroides
spp., as well as
H.influenzae, S.pneumoniae
, less often
S.intermedius, M.catarrhalis, S.pyogenes
.
Isolation of S.aureus
from the sinus is characteristic of nosocomial sinusitis.
Choice of antimicrobials
Drugs of choice
: amoxicillin/clavulanate. For nosocomial infection - vancomycin.
Alternative drugs
: cefuroxime axetil, co-trimoxazole, ciprofloxacin, chloramphenicol.
Duration of therapy
: 10 days.