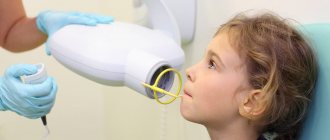
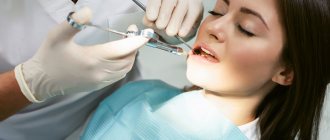
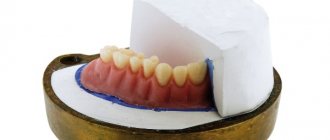
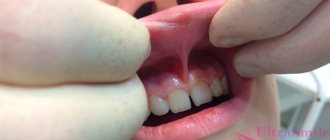
Physics and medicine
Without air, a person cannot live even for a few seconds. This natural mixture, many gases, as well as their absence - vacuum, are widely used in human life. For example, in medicine and some areas of production, aspiration sampling is used. In medicine, this term refers to several concepts:
- a procedure that allows you to collect material using a vacuum;
- a physiological process based on the “suction” effect that occurs due to a decrease in pressure.
In the article we will consider another concept used in medical practice, called aspiration test. As a physical phenomenon, aspiration is the process of sucking air through special instruments or devices, which is then studied and analyzed for the content of substances in the material under study.
The meaning of the test
In medicine, an aspiration test is used for self-monitoring of medical personnel during manipulations, for example, when administering an injection, as well as when removing biomaterial for further study. Used in ecology, sanitary and epidemiological control and in industry, the aspiration method of air sampling allows for analysis of gas or liquid. The aspiration technique is simple and in many cases does not require complex equipment. By drawing the material under study into special equipment using an artificially created vacuum, a specialist can even visually, if provided for by the operating algorithm used, determine the presence or absence of certain inclusions. Air sampling using the aspiration method is a quick and fairly informative way to obtain the necessary information about the composition and quality of the gas. In medicine, aspiration of biological fluid allows competent and high-quality self-monitoring of a medical worker when administering injections. After all, drug delivery must be carried out in a certain way: some drugs must enter directly into the blood, other substances must be delivered intramuscularly. It is the process of correct injection that allows monitoring the aspiration test.
Anesthesia
Self-monitoring of aspiration during procedures has become widespread among medical professionals, because parenteral administration of drugs is used in almost all areas of medicine. Anesthesia is no exception. The drug must act in a certain way depending on the assigned tasks. An anesthesia aspiration test is a method of monitoring before administering a drug by injection to ensure that the syringe needle is positioned correctly to obtain the desired result. Local work of the anesthetic substance is ensured by its introduction into the extravascular space. This is precisely what can be determined by preliminary sampling of the environment from the place where the needle with the active component hit.
Types of local anesthesia
Infiltration anesthesia is most often used in dentistry. It involves injecting an anesthetic with a thin needle under the mucous membrane next to the problem tooth or inside the bone, which begins to act 10 minutes later. The resulting effect lasts for 2–3 hours, depending on the drug used, the depth of its administration and the amount.
Another type of anesthesia is application. It is used quite rarely and can relieve pain only with shallow interventions. In this case, various ointments and sprays are used, which are applied to the desired area with a sterile cotton swab or gauze.
This technique is best suited for cases such as:
- treatment of superficial caries;
- removal of tartar;
- anesthesia of the area before another anesthesia (deeper);
- installation or removal of a crown;
- manipulation at the edge of the gum.
The third method of local anesthesia is the use of conduction anesthesia. It stops the transmission of nerve impulses for some time. This method is based on the administration of an anesthetic through the branches of the trigeminal nerve. Relief from painful sensations occurs within 2–3 hours. The technique of performing such anesthesia is somewhat more complicated than others. It is recommended mainly for the treatment and removal of molars (large molars) or intervention in the gums.
Trunk anesthesia is very rare in dental practice; it is justified only by obtaining a long-lasting effect. Its essence lies in the introduction of special drugs using a thin needle at the base of the skull that block the maxillary and mandibular nerves. Such anesthesia is most often performed during major operations in a hospital setting and in the case of clearly defined pain syndrome.
These are the main types of anesthesia in dentistry, which allow you to take care of dental health relatively painlessly and without much discomfort.
Free consultation
30-40 minutes
inspection and diagnostics
treatment plan and cost
Make an appointment
Dentistry
An aspiration test in dentistry is a technique that allows you to assess the quality of the upcoming anesthesia. In dentistry, there are quite a few types of anesthesia administration; they differ both in the method of delivering the analgesic and in the place of its administration. But in any case, an aspiration test should be a mandatory preliminary procedure. Dental anesthesia should not enter the bloodstream and spread to nearby tissues and organs. Its goal is local work, providing pain relief during the procedure in a small area of the oral cavity. In dental practice, special syringes are used that have not only all the classic details of this instrument, but also special devices on the piston to properly hold it when creating forward and backward movements. At the moment, performing an aspiration test in dentistry using a carpule syringe is considered the most convenient and technologically sophisticated way of both administering an anesthetic and assessing the correctness of the manipulation.
- home
- >
- articles
Pain relief in permanent makeup.
Adverse reactions, complications, treatment tactics.
Ph.D.
Bezugliy A.V., permanent makeup school “Nautilus”, St. Petersburg Issues related to pain relief for permanent makeup have long been regularly discussed at conferences and specialized literature. Despite the short duration of the anesthesia procedure, which takes minutes, it is the most dangerous in terms of the severity of possible complications.
What factors should a permanent makeup specialist consider when choosing an anesthesia method:
- level of own professional qualifications and manual preparedness;
- the presence and properties of local anesthetics, the regulated procedure for their use;
- anamnestic data (allergy history);
- the client's health status (presence of renal and liver failure, circulatory failure, presence of cancer, nutritional disorders (hypoproteinemia), blood pressure level before the procedure, epilepsy or other seizures, etc.);
- correspondence of the duration of action of the selected anesthetic to the duration of the procedure.
Modern pharmacology offers a wide range of pain relief products in cosmetology. How to make the right choice, how to select a drug for a specific client, how to evaluate the effectiveness and predict the duration of anesthesia, what criteria are used to judge the complicated course of pain relief, etc.?
In an ideal situation, a local anesthetic should have low toxicity, a rapid onset of analgesic effect, a predictable duration of anesthesia, a small number of adverse reactions, low allergenicity, etc.
In order to choose the right drug for anesthesia, taking into account the individual characteristics of a particular person, a brief excursion into the course of pharmacology is necessary. Today, about 100 local anesthetics are used more or less actively in medical practice. Moreover, according to their chemical structure, they are all divided into esters (amino esters) and amides (amino amides). The first include novocaine (procaine), tetracaine (dicaine), benzocaine (anesthesin), etc., the second - lidocaine, trimecaine, pyromecaine, mepivacaine, prilocaine, articaine, bupivacaine, etidocaine, ropivacaine, etc. At the same time, promising modern local anesthetics are being developed today based on lidocaine, mepivacaine, articaine and bupivacaine, which are approaching ideal properties in their properties. The different chemical structures of the two groups of anesthetics determine differences in properties, such as toxicity, speed of onset and duration of anesthesia, allergenicity, etc.
Toxicity is inversely correlated with protein binding. The lower the binding of the anesthetic to plasma proteins and the lower the level of plasma proteins, the more pronounced the toxic effect of the drug.
The speed of onset and severity of pain relief are associated with the ability to diffusion - fat solubility. The more anesthetics dissolve in fats, the faster they cross the cell membrane of the nerve and are more effective.
The duration of anesthesia is also directly correlated with protein binding. The higher this indicator, the longer the anesthesia. In addition, the duration of anesthesia depends on the vasodilating properties of local anesthetics. Average “clinical” concentrations of a number of local anesthetics cause dilation of blood vessels, thereby accelerating the absorption of these drugs into the bloodstream and reducing the activity and duration of the analgesic effect. A comparatively more pronounced blood supply to the soft tissues of the face leads to the same effect.
Allergenicity. During metabolism, esters decompose to para-amidobenzoic acid, the substance that most often causes allergies. Amides do not reach this stage of metabolism, so they are much less allergenic. It should be noted that not only the breakdown products of local anesthetics cause allergic reactions, but also additional components used to stabilize anesthetic solutions in the external environment cause allergies.
Components of anesthesia drugs. Using the example of the drug Scandonest 2% SP from Septodont (France) (cited from Kononenko Yu.G., Rozhko N.M., Ruzin G.P., 2008), we can discuss the influence of various chemical compounds on the development of adverse reactions during anesthesia. Composition of the drug: mepivacaine hydrochloride, 36 mg (2% mepivacaine), adrenaline, 18 mg (adrenaline 1: 100000), potassium metabisulfate, 2.16 mg (antioxidant), methyl parahydroxybenzoate, 1.44 mg (methylparaben), propyl parahydroxybenzoate, 0. 36 mg (paraben), sodium chloride, 1.44 mg (buffer), water for injection up to 1.8 ml. At the same time, antioxidants (sulfites) prevent the oxidation of the vasoconstrictor. They can cause allergic reactions, provoke breathing problems, and an attack of bronchial asthma. Parabens (methylparabens) are antibacterial preservatives used in solutions of lidocaine and mepivacaine. They cause allergies more often than the anesthetic itself. Buffer – equalizes the pH of the drug to reduce pain during its administration. Vasoconstrictors (adrenaline, norepinephrine, vasopressin, felypressin) are added to the anesthetic to prolong and enhance the analgesic effect. The first three can cause a systemic reaction due to a general vasoconstrictor effect. Each of the components presented in the 2% Scandonest solution performs its necessary function, but some of them cause the development of adverse, toxic and allergic reactions.
Classification of anesthesia methods used in permanent makeup:
Terminal: - implies an effect on nerve endings located in intact skin and mucous membranes. The depth of penetration of drugs and the duration of anesthesia, as a rule, do not allow long procedures to be performed. Most often in practice, 10% lidocaine spray and eye drops are used.
Application:
- for intact skin (a high concentration of anesthetics is required, the use of “active” diffusion and a change in the normal barrier properties of the skin using penetrant substances and a number of other pharmacological techniques);
- for damaged skin (passive diffusion of anesthetics through damaged skin is possible; the combined use of “short” and “medium”, “medium” and “long” drugs and the addition of vasoconstrictors to lengthen the time of anesthesia are often used).
This is followed by injection methods of pain relief, the implementation of which is allowed with a higher medical education.
Infiltration: low concentrations of administered drugs are used, there are restrictions on the quantity and frequency of administration of anesthetics, and the use of vasoconstrictors is possible.
Conductor. It is characterized by the possibility of increasing the concentration of the active substance and reducing the volume of the drug, the need to administer the anesthetic at a distance of 2-3 mm from the nerve trunk, an increased risk of developing systemic complications, the importance of technical features - the premise of the solution and an aspiration test.
Characteristics of the drugs most commonly used for
topical anesthesia:
benzocaine (anesthesin, anestalgin) – 5-20% oil solution, 5-10% ointments and creams.
tetracaine – 0.5-2% solutions, creams, gels, ointments.
lidocaine – 5% gel, 2-5% ointment.
prilocaine – 2.5-8%.
infiltration anesthesia:
(the maximum single dose is presented in absolute numbers,
can also be calculated in mg/kg body weight)
novocaine – 0.5-1% solution (maximum single dose – 800 mg (800 ml of 1% solution)).
trimecaine – 1% solution (maximum single dose 1000 mg (1000 ml 1% solution)).
lidocaine – 0.5-1% solution (maximum single dose 200 mg (20 ml of 1% solution)).
conduction anesthesia:
containing 0.5% bupivacaine (vasoconstrictor - adrenaline 1: 200000):
- marcaine.
containing 4% articaine (without vasoconstrictor, adrenaline 1: 100,000 or 1: 200,000):
— ultracaine DS and DS forte;
— septanest 4% SP, N, SVC;
— ubistezin and ubistezin forte;
- alfacaine N and SP.
containing 2% and 3% mepivacaine (without vasoconstrictor, adrenaline
1 : 100000 or norepinephrine 1 : 100000):
— scandonest 2% SP, NA, SVC;
- mepivastezin;
— mepidont 3%.
containing 2% lidocaine (without vasoconstrictor, adrenaline 1: 50000,
1: 80000, 1: 100000 or norepinephrine 1: 25000):
— xylonor 2% NA, SVC;
— lignospan standard, forte and SP;
- xylostesin A.
Precautions to reduce the risk of adverse reactions during anesthesia:
1) Carefully read the annotation for the drug:
- name of the drug, active substance and additional components;
- permitted method of use (externally, intradermally, subcutaneously, intravenously, etc.);
- dosage in mg/kg body weight for various methods of administration;
- recommended exposure time for external use of the drug;
- combination with other drugs;
- features of use against the background of various diseases;
- contraindications for use;
- reported side effects;
- therapeutic breadth and signs of overdose, etc.
2) suitability of the drug for use:
- integrity of container and closure;
- the presence of clear inscriptions on the walls of the container or stickers;
- mandatory presence of a distinguishable release date and expiration date;
- uniformity of the dosage form;
- absence of sediment and foreign inclusions, etc.
3) Identification of allergies to the drug used:
- allergy history (not only to the commercial name of the drug, but also to its main components);
- performing an intradermal drug tolerance test should be carried out, incl. at your request in the treatment room of a medical institution or in laboratory services using the in vitro method;
- the presence of allergies (urticaria, Quincke's edema, anaphylactic manifestations, dermatitis, etc.) entails the inevitable cancellation of the entire group of “compromised” drugs (ether or amide) and replacing them with the opposite;
- In patients with a history of allergic reactions, drugs that do not indicate the active pharmacological substances should not be used.
Common complications of local anesthesia
- fainting is an acute vascular insufficiency with a short-term disturbance of blood circulation in the brain. The development is often gradual, accompanied by general weakness, dizziness, ringing in the ears, and nausea. Pale skin and cold sweat are noted. Full restoration of consciousness occurs within a few minutes.
- collapse - a more pronounced picture of acute vascular insufficiency, in which signs of a sharp decrease in blood pressure and peripheral circulatory disorders prevail;
- toxic reaction to anesthetic solution:
a) mild toxicity is accompanied by dizziness, tinnitus, and numbness around the mouth. Possible confusion, nausea, decreased blood pressure, increased heart rate, and slight respiratory depression.
b) with moderate severity, twitching of the facial muscles, generalized convulsions, vomiting, tachycardia, a pronounced decrease in blood pressure, and breathing problems are noted.
c) the clinical picture of severe toxic lesions is characterized by loss of consciousness, respiratory arrest, deep arterial hypotension, and cardiac dysfunction.
- allergic reaction (immediate hypersensitivity, delayed hypersensitivity);
- provoking an epileptic attack or other variants of convulsive seizures - the clinical picture is similar to a fainting state, but in addition, as a rule, convulsions, tongue biting, foam at the mouth, involuntary urination and defecation are observed;
- erroneous intravascular administration of the drug: inadvertent intravenous or intraarterial injection may lead to signs of systemic toxicity. Most often, signs of systemic toxicity are associated with symptoms of nervous system damage. When certain concentrations are exceeded, convulsive readiness increases, muscle twitching and clonic-tonic convulsions appear.
Local complications of injection anesthesia
- accidental damage to blood vessels may be accompanied by the formation of hematomas or external bleeding. More often, such complications occur in patients with slow blood clotting. Either due to blood diseases (hemophilia, deficiency of blood clotting factors), or in cases of taking antiplatelet agents and anticoagulants;
- Ischemia of facial areas can occur in cases of superficial subcutaneous administration of anesthetics containing vasoconstrictors. The areas of skin over the area of incorrect administration of drugs appear white due to their bleeding. The return of normal skin color occurs 1-3 hours after the injection;
- purulent-inflammatory complications - as a consequence of violations of asepsis rules during execution, develop within 2-3 days. First, edematous-infiltrative stages (inflammatory infiltrates) are observed, then they melt with the formation of abscesses and phlegmons. Less common are other forms of purulent-inflammatory complications, such as lymphadenitis, erysipelas, thrombophlephitis, etc.
- nerve damage, post-injection pain, persistent neuralgia: nerve injury with a needle and intraneural injection are the causes of the development of neuropathies and neuralgia, characterized by persistent pain in the nerve projection and paresthesia.
- violation of the technique of administering the drug with a fracture of the needle - lack of skills in performing the injection and sudden movements of a psychologically unprepared client can lead to a fracture of the needle with further migration of the needle fragment.
Anaphylactic Shock Emergency Kit
Mouth dilator, tongue holder, air duct, gastric tube, tourniquet, Ambu apparatus, blood transfusion systems, syringes of 1 ml, 2 ml, 5 ml, 10 ml, 20 ml, scalpel, tweezers, hemostatic clamp, sterile wipes, bandage.
Norepinephrine 0.2% - 1.0; adrenaline 0.1% - 1.0; ephedrine 5% - 1.0; cordiamine – 1.0; caffeine-sodium benzoate 10% - 1.0; korglykon – 0.06% – 1.0; hydrocortisone – 0.125; prednisolone – 0.3; dexamethasone – 0.004; saline solution in ampoules; aminophylline 2.4% - 10.0; no-shpa – 2.0; atropine (platiphylline) 0.1% - 1.0; calcium chloride (gluconate) 10% - 10.0; diphenhydramine 1% - 1.0; tavegil – 2.0; suprastin – 1.0; lasix 1% - 1.0; dibazol 2% - 2.0; ammonia – 1.0, ethyl alcohol. The supply of each drug is at least 5 ampoules. Reopolyglucin – 1 bottle, saline solution – 1 bottle.
The presented set of instruments and medications can only be completed in a medical institution because contains a number of group A drugs that require special storage conditions. In studios and beauty salons, this set can be presented in a shortened version. Providing assistance for anaphylactic reactions should be carried out by specialists with medical education, whose competence includes the necessary amount of knowledge, regardless of specialty.
Scope of first aid: stop the allergen, apply ice to the injection site, place the patient on his back with his legs raised, turn his head to the side, remove the dentures, extend the lower jaw and fix the tongue. Subcutaneously or intramuscularly inject 0.5 ml of a 0.1% solution of adrenaline, 1 ml of a 5% solution of ephedrine, provide access to fresh air or inhale oxygen.
First medical aid consists of intravenous drip administration of 1 ml of 0.1% adrenaline solution (1 ml of 0.2% norepinephrine solution) in 400 ml of 0.9% sodium chloride solution. With low blood pressure, the rate of drug administration is increased. 100 mg of hydrocortisone (90-120 mg of prednisolone), 1-2 ml of 1% diphenhydramine solution are administered intramuscularly or intravenously.
Various clinical variants of the course of anaphylactic shock (arterial hypotension, bradycardia, edema of the upper respiratory tract) require supportive and symptomatic therapy.
Modern drugs used for topical anesthesia:
Containing only amide preparations: 5% emla cream (lidocaine, prilocaine), anestop (prilocaine).
Containing ether and amide preparations: super trio (lidocaine, tetracaine, benzocaine), sustain (lidocaine, tetracaine), eyz-a-blue (lidocaine, tetracaine), prepcain (lidocaine, tetracaine), blue ice (lidocaine, tetracaine), meso numb (benzocaine, tetracaine, lidocaine), etc.
Upcoming courses in St. Petersburg:
https://www.pm2000.ru/services/
Cosmetology
Aesthetic medicine is developing rapidly. But a procedure such as injection remains the most common way of introducing medications and cosmetics into the subcutaneous and deep layers of the epidermis. This procedure has the potential for tissue embolization. In order to avoid the adverse consequences of the intervention, an aspiration test is performed in cosmetology. What kind of manipulation is this? Its purpose is to control the correct placement of the medical instrument to obtain a high-quality result with minimal complications. When carrying out an intervention, the specialist must take into account many factors, one of which will be the individual scheme of the patient’s vascular system. Therefore, a test to verify the correctness of the procedure is simply necessary. For example, if during the procedure for introducing a gel into the subcutaneous layer, the active substance enters a blood vessel, this will cause a disruption of blood flow, and then ischemia and necrosis. In addition, in some cases, retrograde injection of a special material is indicated, which also involves the use of aspiration.
Artery embolization in cosmetology: how to prevent the irreparable
Safety issues in aesthetic medicine always remain relevant. Every doctor strives to minimize the risks of complications, and especially those that can lead to irreversible changes.
Intra-arterial injection of gel-like drugs leads to a critical decrease in blood flow in a certain anatomical area, which can cause ischemia and then necrosis.
To limit the risk of embolization, many experts advocate performing aspiration before injection, since blood in the center of the needle during this manipulation will confirm its intravascular location.
Collection of biomaterial
Carrying out medical manipulations may also include the removal of a cytological sample for examination. An aspiration test also helps with this. The need for a biopsy, for example, is determined by the doctor. Often this procedure is carried out simultaneously with other diagnostic measures, for example, bronchoscopy, colonoscopy, and so on. The collection of tissues or liquids necessary for analysis is carried out either with a syringe or with an aspiration gun - a more powerful design intended only for these purposes. The cytological sample is then delivered to the laboratory for examination, so the sampling procedure is the most significant stage of the biopsy.
Advantages
Aspiration biopsy has become widespread due to the following set of advantages:
- low morbidity, high safety, simplicity of method
- the procedure does not require hospitalization of the patient
- pipel is a disposable instrument, so its use eliminates the risk of infection
- the outer diameter of the instrument does not exceed 4.5 mm, so the procedure, unlike classical endometrial aspiration, does not require painful expansion of the cervical canal
- low risk of inflammatory complications
- The technique allows tissue sampling from any part of the uterine cavity
- a relatively inexpensive method, the effectiveness of which increases significantly if regular examination of the endometrium is necessary, for example, in cases of infertility caused by hyperplastic and hormonal processes
Microbiology
Particular importance is attached to such procedures as the aspiration method of air sampling, microbiology. Science that studies the inhabitants of the microworld helps many areas of knowledge and human activity to develop, taking into account and using the characteristics of the life of microorganisms. Aspiration samples of air intake are widely used in sanitary and epidemiological control. Moreover, the collection of material is the most critical stage, the correct execution of which determines the quality of the analysis performed. An aspiration test in this case is a forced method of deposition of microorganisms from the environment onto a nutrient material or a special collecting liquid. This way, experts can monitor their growth and conduct research.
Sample collection techniques in medicine
In medicine, the same syringe used for injection is used as an aspiration device. The basic principle of operation of instruments and devices for carrying out aspiration manipulation is vacuum suction of the medium. For example, the reverse movement of the syringe piston, which creates negative pressure.
The technique for monitoring the correctness of the injection recommends following the following algorithm:
- The plunger of the syringe, already in the working position, must be pulled back gently, without applying excessive force.
- The piston stroke can be only 1-2 millimeters to obtain sufficient aspiration vacuum.
- It is unacceptable to change the position of the syringe both during the aspiration test and during the injection. To do this, it is fixed using a stop with the ring finger and little finger of the medical worker performing the procedure.
- If the needle is thin, it may take a few seconds for the test results to appear. If the test is positive (which depends on the expected result), then the injection is placed in place without displacing the needle. If the test result is negative, then the needle is either moved a few millimeters without removing it from the tissue, or the injection site itself is changed.
When injecting into a highly vascularized area, multiple aspirations may be required to determine the optimal location for the procedure.
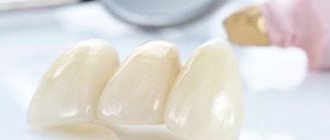
Carpule anesthesia
Carpule anesthesia is anesthesia that uses a special syringe. It is used for comfortable and safe anesthesia. In modern dentistry, this method of pain relief is considered one of the most popular. It costs more than usual, but, according to reviews, it is very easy to carry, and the process of inserting the needle is practically not felt.
Carpule syringe in dentistry
Carpule syringes in dentistry are disposable dental injectors that are equipped with a system to protect against accidental needle injury. Also, a carpule syringe has a needle, a piston part and a base body. In the side of the body there is a place for inserting a carpule.
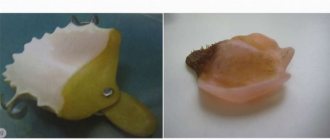
Carpula is a special container containing an anesthetic substance. On one side of the container there is a rubber stopper, on the other there is a metal lid.
The difference between a carpule syringe and a classic one is as follows: the piston of the system cannot be removed by moving it backwards, as in conventional analogues.
The system works as follows: the desired carpule with anesthetic is placed in the syringe, a disposable carpule needle is attached, and it is inserted into the area in need of anesthesia.
Today, all leading dentists use precisely such solutions for administering anesthetics. The syringes are technically sophisticated, comfortable to use, and most importantly, the patient does not feel pain during the piercing of living tissue and the administration of anesthetic.
Pros and cons of carpule anesthesia
- allows you to accurately measure the volume of injected anesthetic. Each carpule is designed to hold 1.7 ml of anesthetic substance, which makes it easier to control the substance and not exceed it. Each capsule contains the name of the anesthetic, the dosage, and the introduction of other substances is excluded;
- absolute sterility - the solution inside the carpule is introduced in compliance with the rules of sterility, and the needles used are strictly disposable;
- flexible needle – this feature has already been appreciated by dentists. Unlike classic syringes, the needles in carpule syringes bend well, do not break off, and there is no chance of debris getting into tissues or wounds;
- comfort when working as a dentist - it is much more convenient for a specialist to work with a compact and technically sophisticated carpule device, the needle is correctly placed in the tissues for a successful injection;
- ultra-thin needles - thanks to their special shape, the needles are easily inserted into the tissue, and the patient practically does not feel them.
For comparison, previously the dentist mixed several substances for pain relief, which required a lot of experience and effort. There is a risk of complications when mixing medications yourself.
Among the disadvantages of this type of anesthesia, we note its considerable cost (such syringes are more expensive than simple analogues), as well as the inability to mix the anesthetic, since the substance is already sealed in the carpule.
Carpule anesthetics
There are modern anesthetics in dentistry designed specifically for carpulal anesthesia. The most common options:
- Carpules with ultracaine are a product produced in France, which is presented in three varieties (depending on the volume of the substance epinephrine included in its composition). Ultracaine in dentistry is one of the most popular carpule anesthetics, well tolerated by patients, and has a minimum of contraindications;
- Scandonest in dentistry is another common anesthetic produced in France, which contains the substance mepivacaine. It does not contain vasoconstrictors, and therefore is used for patients in the so-called “risk group” (who have been diagnosed with bronchial asthma, have an allergy or individual intolerance to adrenaline, epinephrine). An analogue of this drug is mepivastezhin 3 produced in Germany;
- Septanest in dentistry is an anesthetic with the active ingredient adrenaline. It is produced in several variations, depending on the amount of adrenaline content. Contraindicated for people with bronchial asthma and allergies to adrenaline;
- ubistezin is an anesthetic, which is presented in carpules. Means of production in Germany. Ubistezin contains the potent substance epinephrine; the anesthetic is an analogue of ultracaine.
Painkillers should be stored in a dry, cool place at a temperature of 25 ° C.
Which anesthetic is better to choose?
Basic requirements for anesthetics:
- absence of toxic substances in the composition;
- low likelihood of adverse reactions;
- rapid excretion from the body;
- absence of an allergic reaction in the patient.
The choice of anesthetic is made by the dentist based on the indications and general health of the patient. Before administering the anesthetic, it is recommended to do allergy tests to avoid unpleasant situations.
Dentists at 32 Dent actively use carpule anesthesia when treating their patients. Make an appointment with a dentist who will offer optimal treatment for your existing dental problems using carpule anesthesia.
If you have a problem similar to that described in this article, be sure to contact our specialists. Don't diagnose yourself!
Why you should call us now:
- We will answer all your questions in 3 minutes
- Free consultation
- The average work experience of doctors is 12 years
- Convenient location of clinics
Single contact phone number: +7
Make an appointment
Analysis Tools
Carrying out manipulations to collect material and monitor the expected results requires the use of special tools or devices. In medicine, such a tool is a syringe with a needle. For example, aspiration test with a carpule syringe is widely used in dentistry. This instrument can have several design options, which depend on both the carpule itself (a two-chamber flask containing an anesthetic and a medicinal solution) and the design of the piston. The prerogative of such instruments is the aspiration test in dentistry, although the design features, which make it possible to fix both the instrument itself and the movement of the piston (both direct and reverse), are used in many branches of medicine where injections are necessary. Also in practice, a suction gun is used - a more powerful device designed for collecting biomaterials. In medicine, aspiration is not only a purely medical procedure. For example, many parents know what an aspirator is - a special bulb with a nozzle that allows you to remove the contents of the nasal cavity of an infant who cannot yet independently get rid of accumulated mucus.
A wider range of tools is used in other areas of human activity where it is necessary to collect the environment. Air sampling using the aspiration method in sanitary epidemiology is carried out using the following instruments:
- Seitz apparatus;
- Krotov apparatus;
- Rechmensky bacteria trap;
- Andersen devices;
- Dyakonov device;
- air sampling device (POV-1);
- Kiktenko device;
- aerosol bacteriological sampler (PAB-1);
- bacterial-viral electroprecipitator (BVEP-1).
Such an abundance of devices for aspiration in sanitary epidemiology and other fields of science suggests that each of them has its own shortcomings or is not capable of performing a set of functions necessary in each specific case.
An aspirating air sampling device is an instrument or device used in industry or in public health inspections. Depending on the conditions, devices are used to draw in air, filtering its contents for subsequent study or removal.
Devices for aspiration and extraction of solid elements from the air are widely used in workshops, both industrial and amateur. For example, during wood processing, air is taken from under the tool along with chips, which are separated and removed from the workplace.
If you don’t pay too much attention to some features, then any exhaust device that operates on a forced negative pressure can be called aspiration.
Aspiration biopsy - technique
Depending on the purpose of tissue sampling, the study may be prescribed at different periods of the menstrual cycle. Most often, aspiration biopsy of the endometrium is performed on days 21-23. Due to its relative simplicity and minimally invasive nature, the method allows sampling on an outpatient basis.
Pipelle biopsy does not require any special preparatory procedures. The day before performing an aspiration biopsy, it is recommended to stop using vaginal suppositories, ointments, any lubricants and tampons. To reduce discomfort, an anesthetic drug is prescribed an hour before the procedure. For the purpose of pain relief, an anesthetic is applied directly during the procedure to the mucous membrane of the cervix using a spray bottle.
To collect tissue, a sterile disposable instrument is used - a pipel - named after the inventor. This is a flexible, thin plastic tube with a piston that allows you to create negative pressure in the tube. After inserting the instrument into the uterine cavity, the doctor pulls out the piston halfway to create a reduced pressure in the cylinder located at the end of the tube. Due to this effect, endometrial tissue is sucked into it. In this case, both the superficial tissue of the uterine glands and the endometrial tissue are transferred for analysis, which allows for an effective diagnosis of the disease. The material obtained as a result of aspiration biopsy is sent for histological examination. The results of tissue sampling can be obtained a week after the study.
After the procedure, the patient may experience minor nagging pain, which disappears after a few days. Sometimes there is a slight spotting.
Activity factors
An aspiration test is an effective way to monitor the medical procedure being performed, as well as to collect material for further study. Any medical procedure must first and foremost be safe. To assess the risk and effectiveness of aspiration manipulation, the specialist must take into account several factors:
- rheology, that is, fluidity, of the drug and the biomaterial being taken;
- geometric parameters of the needle: its diameter and length;
- the dimensions of the syringe itself, its dimensions and, therefore, the physical capabilities of creating back pressure;
- aspiration time;
- back pressure value;
- patient's blood pressure.
Result
A positive aspiration test depends on what result is needed to obtain when performing it. When performing an intravenous injection, a test is considered positive if the result is the presence of a small amount of blood in the syringe. This means that the needle is intravascular. However, such testing is not always completely adequate, therefore, when carrying out certain medical procedures, for example, when “pumping” silicone or other liquids into the layers of the skin, care must be taken so that the procedure does not result in tissue embolization, which can lead to serious complications, even necrosis.
Why aspiration test cannot be a safety criterion
There are a huge number of factors that influence the effectiveness of aspiration, the most significant are:
• rheology of the drug;
• needle size (diameter, length);
• syringe dimensions;
• aspiration time;
• negative pressure created during aspiration;
• blood pressure.
The specificity of the aspiration test is high, since the appearance of blood indicates a very high probability that the needle is intravascular. However, the sensitivity of aspiration as a diagnostic test is low because the absence of blood does not preclude the possibility of intravascular placement of the needle tip.
What volume of filler leads to artery embolization
Studies have shown that the average volume of filler, the introduction of which into a vessel leads to embolization of the artery, is approximately equal to 0.08 ml, however, blockage of the vessel can occur with the introduction of only 0.04 ml. Therefore, the maximum injected volume should not exceed 0.04 ml per bolus when injecting with a needle, given the possibility of this complication.
The effectiveness of aspiration depends on differences in the physiochemical structure and rheological properties of the fillers.
The higher the density of the dermal filler, the greater the likelihood of a false-negative aspiration test result.
How to avoid complications after minimally invasive cosmetic procedures