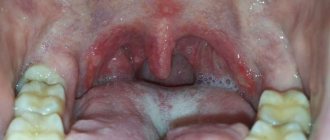
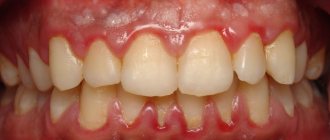
Causes of redness in the throat
In most cases, redness of the mucous membrane of the throat is combined with pain when swallowing and occurs as a result of the development of tonsillopharyngitis1. Isolated damage to the pharynx (pharyngitis) and pharyngeal tonsils (tonsillitis) is rare, and there is nothing surprising about this: the pharynx and tonsils are located close to each other1,2,4.
Most often, inflammation of the pharynx is accompanied by acute respiratory infections (ARI). In preschool children, in 89% of cases, ARI is caused by viruses 1. The mucous membrane of the pharynx and tonsils is a favorite place for rhinoviruses and adenoviruses, as well as parainfluenza viruses. Less commonly, its inflammation is caused by the Epstein-Barr virus, enterovirus (Coxsackie virus), and herpes simplex virus1,2,5.
The viral nature of tonsillopharyngitis predominates in children aged 1 to 5 years3. Starting from the age of five, children more often suffer from bacterial forms of the disease. Moreover, in 20-30%1,2,4,5,7 (according to some data, in 75%3) of young patients, doctors find a dangerous bacterium in the throat and tonsils - beta-hemolytic streptococcus of group A2,3,4,5,6 .
Other microbes can also cause redness in the throat: mycoplasma, chlamydia, staphylococcus and Candida fungi2,3. Sometimes tonsillopharyngitis becomes one of the manifestations of a general disease2,3: diphtheria, scarlet fever, infectious mononucleosis, tularemia, typhoid fever or even HIV3. Treatment will be different in each case.
Types of dry cough in children
Dry coughs range from minor coughing to poorly controlled attacks. The following types of cough are distinguished:
- Acute - appears suddenly, most often accompanies viral infections, foreign body entry into the respiratory tract.
- Protracted - may be the result of an acute cough, usually appears during a period of prolonged recovery after ARVI or acute bronchitis, lasting more than 4 weeks
- Chronic - develops after three months (12 weeks) of prolonged cough; it can be a complication after an untreated disease.
- Paroxysmal - appears as an uncontrolled attack, may be a symptom of an allergic reaction or whooping cough.
- Barking is often a symptom of laryngitis, laryngotracheitis, and inflammation of the larynx. It may be a manifestation of false croup, a dangerous condition in children.
Symptoms to watch out for
The development of tonsillopharyngitis in a child is difficult to miss. Children are extremely sensitive to sore throats1,5,6. With its appearance, babies' sleep and appetite are disrupted, they become capricious and whiny1,6. Older children complain of a sore throat and sore throat when swallowing6,7. They develop a dry, superficial cough1,7.
A runny nose, red throat and fever in a child, especially in the autumn-winter period and early spring, most often indicate a cold, that is, ARVI1. The mucous membrane of the pharynx looks reddened, swollen, loose, dry or moist, covered with cloudy mucus1,2.
With an adenovirus infection, these symptoms include redness of the white membrane of the eyes, swelling of the eyelids, lacrimation, and “films” typical of adenoviral conjunctivitis appear in the eyes. 1.2. Lymph nodes enlarge. Sometimes nausea, vomiting and abdominal pain occur1. Upon examination, the pharyngeal mucosa appears slightly reddened, loose, with whitish deposits and lumps of thick mucus1,2.
The development of tonsillopharyngitis may be associated with enterovirus infection caused by Coxsackie viruses1,2. Enteroviral vesicular pharyngitis is called herpetic sore throat, since the rash resembles the blisters of herpes 2. Blisters filled with cloudy liquid appear on the reddened mucous membrane of the pharynx and oral cavity, and even on the plantar surface of the feet and palms. Possible muscle and abdominal pain1.
Fever, red throat and cough in a child may be manifestations of infectious mononucleosis associated with Epstein-Barr viruses1,2. In this case, in addition to redness and swelling of the mucous membrane of the pharynx, purulent “films” on the tonsils, all lymph nodes, liver and spleen are also enlarged1,2.
Tonsillopharyngitis caused by beta-hemolytic streptococcus is considered the most dangerous form of the disease2,3. This is due to the large number of complications that infection2 can lead to if it is not treated or treated incorrectly.
Streptococcal tonsillopharyngitis sometimes leads to the development of peritonsillar abscess, rheumatic fever, glomerulonephritis, and bacterial endocarditis2.
The following symptoms will help you suspect that redness in the throat is the result of the activity of streptococci:
- high temperature (> 380 C);
- absence of runny nose and cough;
- severe sore throat, forcing you to refuse food;
- severe swelling of the tonsils;
- the appearance of pinpoint hemorrhages (petechial rash) on the mucous membrane of the tonsils, soft palate and pharyngeal walls;
- purulent plaque on the tonsils, tightly connected to the underlying tissues;
- the appearance of ulcers and erosions on the tonsils in places where plaque is rejected;
- enlarged cervical lymph nodes2,3,7.
If a child has a red throat, but no temperature, this is a reason to think about non-infectious causes. Redness of the pharyngeal mucosa in a baby can be caused by prolonged crying, staying in a smoky room, eating too cold or hot food, or trauma to the pharynx with sharp objects. Sometimes the mucous membrane is colored red by dyes found in foods. The doctor takes all this into account when diagnosing tonsillopharyngitis1,2.3.
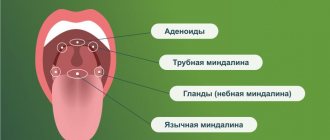
Anatomical structure
The oropharynx is a continuation of the nasopharynx, the middle section of the larynx. It starts from the hard palate and ends at the entrance to the larynx. The organ is connected to the oral cavity by the pharynx, and is separated by the palatine arches, soft palate and dorsum of the tongue. In this section the digestive and respiratory tracts intersect. The oropharynx contains:
- the back third of the tongue (its root);
- tonsils;
- posterior and lateral walls of the pharynx. The posterior wall is located at the level of the third cervical vertebra. The side walls connect to the eustachian tubes of the ears.
What to do if a child has a red throat?
A red throat as a symptom is very rarely isolated. It is accompanied by other signs that add up to one or another clinical picture. Only a doctor can correctly assess it and select adequate treatment. Therefore, if your child’s throat is red, you should definitely visit the children’s clinic.
Which doctor should I contact? Of course, to the pediatrician. If necessary, he will refer you to the right specialist, an infectious disease specialist or an ENT doctor.
Treatment of tonsillopharyngitis, which is prescribed by doctors, usually includes general and local therapy. If the disease is caused by bacterial microflora, antibiotics are used1,2,7. For viral infections there is no point in using them: viruses are not sensitive to these drugs2,4,5,7.
Antipyretic drugs based on paracetamol and ibuprofen2,4 approved for children are used as needed, mainly when the temperature rises above 380 C and/or poor heat tolerance1,3.
In local therapy, drugs based on antiseptics1,3,4 are widely used - substances with antimicrobial effects. Preference is given to those forms that are easy to use and have a pleasant taste, which is especially important for children1,5,6.
For local treatment of inflammatory diseases of the pharynx in children over 3 years of age, depending on age, HEXORAL®2,3,4,5,6 preparations can be used. Aerosols and lozenges are especially convenient6,7.
HEXORAL® aerosol with mint flavor is approved for use in the treatment of children over 3 years of age8. It is based on the antiseptic hexetidine, which has a wide spectrum of antimicrobial action, is active against some viruses, and can have a mild analgesic effect8. A convenient bottle with a nozzle allows you to spray the drug evenly over the entire surface of the pharynx.
If a child is over 3 years old and already knows how to gargle, HEXORAL®11 solution can be used for the rinsing procedure. In addition, the solution is suitable for treating the throat with a tampon.
HEXORAL® tablet forms are distinguished by a variety of tastes.
“Mint” HEXORAL® TABS based on the antiseptic chlorhexidine and the local anesthetic benzocaine can complement the traditional therapy of tonsillopharyngitis in children 4 years of age and older9.
HEXORAL® CLASSIC with the flavors of orange, lemon, black currant, lemon and honey with lemon is suitable for children over 6 years old10.
Adolescents over 12 years of age are allowed to use HEXORAL® EXTRA tablets, which, in addition to the antiseptic component, contain the anesthetic lidocaine, which can relieve even severe sore throat12.
If your child is sick, you should consult a pediatrician in any case. Only he is able to determine how to treat the baby, because a red throat can be a symptom of a serious disease.
The information in this article is for reference only and does not replace professional advice from a doctor. To make a diagnosis and prescribe treatment, consult a qualified specialist.
to come back to the beginning
Literature
- I. N. Zakharova, E. B. Machneva. Pediatrician tactics for acute tonsillopharyngitis in children. Medical Council No. 1, 2022 pp. 128-132.
- Zaitseva S.V., Zastrozhina A.K., Kulikova E.V. Acute tonsillitis in the practice of a pediatrician. Medical advice. 2019; 2: 113-119.
- G. A. Samsygina. Acute tonsillopharyngitis in children. Pediatrics2008/Vol. 87/No. 3 pp. 91-95.
- S.A. Karpishchenko, S.I. Alekseenko, S.V. Baranskaya. Treatment of tonsillopharyngitis in children // Medical Council, No. 1, 2022, pp. 70–75.
- Karpishchenko S.A., Lavrenova G.V., Alekseenko S.I., Muratova E.I. Issues of choosing drug therapy for sore throat in children. Pediatrics (Appendix to the journal Consilium Medicum). 2018; 1:39–42. DOI: 10.26442/2413-8460_2018.1.39-42.
- HELL. Vetrova. Acute tonsillitis in children: a pediatrician’s point of view // Pediatric pharmacology. 2014; 11 (2): 61–64.
- Piskunov V.S., Nikitin N.A. Symptomatic treatment of tonsillopharyngitis in acute respiratory viral infection in frequently ill children. Pediatrics. Consilium Medicum. 2019; 1:44–51. DOI: 10.26442/26586630.2019.1.190192.
- Instructions for use of the drug HEXORAL® aerosol: .
- Instructions for use of the drug HEXORAL®TABS: .
- Instructions for use of the drug HEXORAL®CLASSIC: .
- Instructions for use of the drug HEXORAL® SOLUTION: .
- Instructions for use of the drug HEXORAL® TABS EXTRA: .
Diagnosis of cough
Most often, cough is a symptom of respiratory diseases, the diagnosis of which is not difficult for a doctor. Based on the results of the examination, the specialist will determine the fact of ARVI.
A dry cough in a child without snot and fever requires more extensive diagnostics. A chest x-ray can help here, and if necessary, a specialist will refer you to a CT scan.
Fiberoptic bronchoscopy, or video bronchoscopy, is a method that can be of great importance in identifying complex and hidden causes of cough. It allows you to visually assess the patency of the bronchi, the condition of the mucous membranes, and also obtain tissue and sputum samples for further study in the laboratory.
Spirography is a method for studying the functioning of the respiratory system. It helps to assess the function of external respiration and get an idea of how fully the respiratory system works. Blood gas testing is necessary to diagnose respiratory failure.
Radiopulmonography is used to detect uneven ventilation, which is caused by narrowing of the small bronchi.
An ECG is needed to assess the function of the cardiovascular system, since sometimes heart disease is the cause of a dry cough in a child . Also, with pulmonary hypertension accompanied by a cough, there is a risk of developing heart complications.
Laboratory tests are carried out without fail. A general blood test helps the doctor draw conclusions about the activity of the inflammatory process. Since with a dry cough it is impossible to collect sputum for analysis, examination of the contents of the bronchi can only be carried out after bronchoscopy.
Features of the treatment of dry cough in children
Treatment of dry cough in a child is carried out comprehensively. It is important to follow several recommendations that are relevant for any cause and case of dry cough:
- Schedule. The regime can be bed or semi-bed depending on the child’s condition, but it is important to ensure sufficient sleep and rest. It is advisable to go to bed and get up at the same time; if necessary, add a nap during the day.
- Walks. Fresh air is of great importance in recovery. If you are feeling well, it is important to take a walk every day.
- Ventilation and humidification of the air in the room.
- Drink plenty of fluids. Warm drinks moisturize the mucous membranes of the oropharynx, and a sufficient amount of liquid is necessary to remove toxins and change the consistency of sputum.
Drug treatment is aimed mainly at eliminating the causes of dry cough in children, as well as restoring the normal functioning of the respiratory system. Antibiotics are recommended only in cases with an established bacterial infection; they are not prescribed for ARVI.
the child’s dry cough is of an allergic nature, medications with antiallergic effects are prescribed.