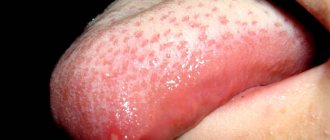
Stomatitis is an inflammation of the mouth (but can also develop on the tongue and lips) that is most often diagnosed in children. Stomatitis in adults is usually a consequence of the introduction of viruses into the oral mucosa. In addition, this disease can occur in the presence of a number of other diseases, due to decreased immunity. For dentists, diagnosing and treating stomatitis in the mouth does not cause any difficulties, while attempts to get rid of the disease on their own can lead to unpleasant consequences
Types of disease
According to ICD-10, aphthous stomatitis is assigned code K.12. Within the code there are three qualifying diagnoses, including K.12.0 - “recurrent aphthae of the oral cavity,” which also includes aphthous ulcers.
According to the form of occurrence, acute and chronic aphthous stomatitis are distinguished. The first is characterized by the appearance of ulcers and severe hyperemia - swelling, redness of the mucous membranes. Severe pain occurs, especially when eating or talking. Submandibular lymph nodes may enlarge and body temperature may rise.
Chronic recurrent aphthous stomatitis may be the result of improper or untimely treatment, as well as the inability of the immune system to cope with the disease. It is characterized by periodic exacerbations. Outside of exacerbation, symptoms may be erased or completely absent.
The disease is classified into three forms depending on the severity:
- light. From 1 to 2 afts up to 10 mm in size. Moderate pain during mechanical action, relapses occur no more than 2 times a year;
- average. Up to 5 aft, the course of treatment takes up to 3 weeks. The pain is quite pronounced, there is an enlargement of the lymph nodes, relapses up to 2 times a year;
- heavy. Multiple aphthae appear, severe pain. An increase in temperature occurs, and symptoms of general intoxication appear. Treatment takes up to a month, relapses occur up to 6 times a year.
Also, according to the form of occurrence, the following types of inflammatory diseases are distinguished:
- fibrous: blood microcirculation in the upper layer of the mucosa is disrupted, aphthae appear, covered with a fibrous film (plaque). Such ulcers heal completely within 14 days. The disease affects the mucous membrane of the lips, the lateral surfaces of the tongue, and transitional folds. This stomatitis recurs up to 3 times a year;
- necrotic. The epithelium is destroyed, the mucosal area dies. Replacement of tissues with normal epithelium takes from 14 to 30 days. This aphthous stomatitis is not accompanied by acute pain; it is usually observed in patients with severe diseases, including blood pathologies;
- grandular. Damage to the ducts of the minor salivary glands occurs. In this regard, aphthae form close to the glands, and drying of the mucous membranes of the oral cavity occurs due to a decrease in saliva production. Ulcerations are painful and heal within 1–3 weeks;
- scarring. Damage to the cavity of the salivary glands leads to the involvement of connective tissue in inflammation. Aphthae are observed both at the location of the glands and on the mucous membranes of the pharynx and palate. The disease develops into large painful ulcers (up to 1.5 cm). Healing takes up to 12 weeks; after the acute process, pronounced scars remain;
- deforming. The most severe form of the disease, which provokes changes in connective tissue. Aphthae heal extremely slowly, which is accompanied by deformation of the palate, lips, and sometimes narrowing of the oral cavity occurs (if aphthae was observed in the corners of the mouth).
Ask a Question
Diet for stomatitis
Proper nutrition plays a vital role in the treatment of diseases, incl. and stomatitis. First of all, it is important to avoid dishes and foods that irritate the mucous membrane - hot, salty, with a lot of spices. You will also have to give up dry food, coarse and hard products, because... they will increase pain. Avoid foods and drinks with a lot of acids (apples, tomatoes, oranges, sour berries, coffee, sour juices) - they not only irritate the inflamed mucous membrane, but also create a favorable environment for the development of pathogens.
With stomatitis, it is difficult to chew food due to pain, so the main part of the diet should be boiled, stewed foods, preferably crushed into a puree. It is better to use meat and fish in the form of minced meat for cooking; replace broth soups with pieces of vegetables and meat with cream soup or puree soup. It is advisable to eat food warm.
Be sure to include vitamins A, B, and C in your diet, either in natural foods or in supplement form. It is recommended to consume soft foods - soft cheeses and cottage cheese, milk and kefir, viscous and semi-liquid porridges. Baby food (purees, curds, yoghurts, puddings, jellies) is well suited. It is better to replace drinks with tea, herbal infusions and clean water.
Causes of aphthous stomatitis
Not all causes of aphthous stomatitis are fully understood. The mechanism of aft formation is often associated with activation of the local immune system - immune cells begin to destroy the epithelium of the mucous membranes, which leads to ulcers.
Local reasons include the following:
- allergic reactions;
- pathogenic microorganisms;
- mechanical damage (biting mucous membranes, injury from sharp edges of fillings or orthopedic, orthodontic structures);
- temperature or chemical influences.
Systemic causes of aphthous stomatitis:
- menstruation, pregnancy in women;
- sudden cessation of smoking;
- enteropathy, celiac disease, malabsorption;
- blood diseases;
- diseases of the immune system;
- lack of vitamins;
- other systemic diseases (lupus erythematosus, Crohn's disease, HIV infection, etc.).
Stomatitis and coronavirus
There is a lot of talk now that many people develop stomatitis due to coronavirus. And so the question arises - how are they connected? It is quite obvious that coronavirus infection greatly weakens the body, undermines the immune defense, and leads to various complications. And with a decrease in immunity, as we know, many dormant infections in the body are activated, which lead to stomatitis. Therefore, it is impossible to consider stomatitis as a symptom of Covid. But it is more logical to look at stomatitis as a concomitant disease that occurs in approximately half of those suffering from coronavirus infection.
After coronavirus, stomatitis can also occur as one of the possible complications. Particularly susceptible to this are those patients who did not closely monitor the condition of the oral cavity, rarely visited the dentist, who had advanced caries or problems with the gums (gingivitis, periodontitis), and tartar deposits. In order to avoid contracting stomatitis after Covid, it is important to regularly and thoroughly perform oral hygiene, brush your teeth, and visit the dentist in a timely manner.
Stomatitis rarely occurs after vaccination against coronavirus. Some patients have a more difficult time with vaccination, so a decrease in immunity may result in a recurrence of stomatitis, especially in those who have had it before or in those who are at risk.
Symptoms of aphthous stomatitis
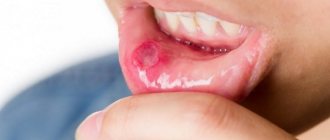
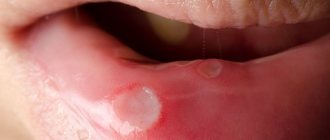
Usually, 1–2 days before the appearance of aphthae, areas of the mucous membrane with increased sensitivity are detected, and a burning sensation may occur. The aphthae themselves are round, have clear boundaries, and are covered with a gray or yellowish coating. Their size, as a rule, does not exceed 1 cm, and the mucous membranes around them turn red.
Such areas of erosion heal within up to 2 weeks without scarring. But in 1 case out of 10, the diameter of the ulcers is more than 1 cm, they affect deeper areas of tissue, and the borders of the pathological area may look raised. Healing in this case takes up to 6 weeks, after which a scar forms.
Aphthous stomatitis is characterized by damage to the mucous membranes of the cheeks, the inside of the lips, the soft palate, tonsils, and the lateral surfaces of the tongue. This is due to the lack of keratinization of the epithelium in these areas. Much less often, aphthae appear on the hard palate, back of the tongue, and gums.
Diagnostic features
At the initial appointment, the dentist examines the oral cavity and analyzes complaints. To make an accurate diagnosis, you need to distinguish this form of the disease from others, as well as differentiate it from other pathologies that have similar symptoms. For extensive lesions, different diagnostic methods may be used:
- clinical blood tests;
- microflora smear;
- blood for PCR to determine the causative agent of the disease;
- biopsy (if indicated).
They are also necessary for recurrent forms of the disease. In simple cases, laboratory diagnostics are not required; aphthae are determined visually by an experienced specialist.
With the help of a comprehensive examination, the doctor will determine which microorganism caused inflammation with subsequent ulceration of the mucous membrane. He also differentiates the disease from herpetic stomatitis and oncological pathology.
Possible complications
If stomatitis in the mouth is left untreated, it will certainly lead to negative consequences, from gum inflammation to tooth loss. That is why it is extremely important when treating stomatitis to strictly adhere to the recommendations given by your dentist. The list of major potential complications includes the following diseases.
- Chronic stomatitis.
Statistically, this is the most common complication. An untreated inflammatory process becomes chronic and recurrent, which means that an infectious focus will always be present in the body. - Appearance of scars.
A symptom such as bleeding gums can be a manifestation of many diseases, but with stomatitis, due to constant non-healing cracks in the oral cavity, scar tissue forms, which in the future may not allow the patient to open his mouth wide. - Laryngitis.
If the infection spreads up the respiratory tract, the patient's voice becomes hoarse and a cough appears. - Vision problems.
With advanced herpetic stomatitis, the target of damage becomes not only the gums, but also the mucous membranes of other organs. Most often, these are the eyes and genitals. - Loss of teeth.
The most dangerous complication of stomatitis. The main threat is the fact that the destructive process can last for many years and may not be noticeable to the patient at first. First, periodontal disease will develop - serious damage to periodontal tissue. And only then, as a consequence, the teeth will gradually become looser until they fall out.
Features of treatment
The main goal of treating aphthous stomatitis is to completely get rid of the disease or at least reduce the frequency of relapses to a minimum. Therapy is aimed at relieving inflammation, relieving unpleasant symptoms, and accelerating the recovery processes of the mucous membrane.
For each specific case, the doctor will develop a set of measures. The main ones include local and systemic drug treatment.
Rinsing with antiseptics can be done using medications or mouth rinses that contain antibacterial components. An alternative to rinsing is to use a spray. Typically, the treatment regimen includes 2-3 sessions of 1-minute rinsing immediately after brushing your teeth.
Local treatment methods include the application of gels with anti-inflammatory and analgesic effects.
Occlusive agents can reduce pain and speed up the healing of mucous membranes. They form an insoluble film on the ulcer, protecting the affected area from exposure to adverse factors.
Local glucocorticoid therapy is used against the background of immune diseases, as well as when standard measures are ineffective. They eliminate pain and quickly relieve inflammation, shortening the healing period. Such products are used only according to indications and are available with a prescription. In some cases, it is advisable to inject the drug under the base of the ulcer; this is done by a doctor.
Epithelialization drugs are used after acute inflammation has resolved. The specialist will prescribe a gel with an analgesic and healing effect, usually this occurs 5–6 days after the start of complex therapy.
Local laser therapy can relieve pain, speed up the healing process, and minimize the risk of relapse.
Systemic treatment of aphthous stomatitis in adults involves taking the following drugs:
- antihistamines (anti-allergic, anti-edematous effect);
- glucocorticoids (anti-inflammatory, analgesic effect);
- immunomodulators (to stimulate defenses and accelerate recovery).
And if antiallergic drugs can be recommended to any patient even in the absence of information about the exact causes of stomatitis, then other drugs are prescribed only according to indications: in case of acute severe course of the disease, frequent relapses, and the presence of severe systemic pathologies. An additional method of treatment is vitamin therapy - taking vitamins C, group B.
In addition to the main course of treatment, all patients without exception are recommended to adhere to a hypoallergenic diet, avoid taking too hot drinks and dishes, and spicy, irritating foods. It is better to give preference to toothpaste without sodium lauryl sulfate, this component can provoke the disease.
It is important to continue your oral hygiene, even if it is difficult. To make brushing your teeth easier, choose a soft toothbrush. If the disease recurs frequently, it is necessary to pay attention to the general state of health, promptly treat teeth and gums, replace fillings and dental structures.
WHY DOES DISEASE OCCUR?
The disease can develop due to:
- infections (in particular, it often occurs during chickenpox, measles, scarlet fever and a number of other airborne diseases);
- oral injuries (for example, cheek biting);
- burns (including after consuming too hot foods or drinks);
- allergic reactions (for example, to medications or dental products);
- insufficient oral hygiene;
- bad habit of chewing a pen or other objects;
- lack of nutrients;
- smoking (this bad habit contributes to the proliferation of bacteria in the oral cavity and constant irritation of the mucous membranes);
- some gastrointestinal diseases (colitis, gastritis and some other diseases can cause the development of catarrhal stomatitis).
Features of treatment in children
The dentist will tell you how to treat aphthous stomatitis in a child. You can contact him at the direction of your pediatrician or on your own if you find characteristic ulcers in the oral cavity. The treatment regimen is the same as that used in the treatment of adult patients, but there are some differences: children under a certain age cannot rinse the mouth, so preference is given to drugs for application to mucosal ulcers. Otherwise, the treatment regimen is developed individually, taking into account the severity, symptoms of the disease, frequency of relapses, and the presence or absence of concomitant ailments in the child. Symptomatic therapy can be used to quickly alleviate the baby’s condition.
Specialists at STOMA clinics successfully treat aphthous stomatitis. By contacting us, you will receive qualified assistance, detailed recommendations on the treatment and prevention of relapse of the disease, and comprehensive assistance from dentists of all specializations, if necessary.
Is treatment possible at home?
Treating stomatitis at home is quite possible, especially if it is not severe. However, it is still necessary to consult a doctor for an accurate diagnosis and choice of medications than to treat stomatitis at home.
To treat herpetic stomatitis at home, local remedies are sufficient: rinsing with miramistin (3-4 times a day) or hexoral. To suppress inflammation, you can use Cholisal gel, for faster healing of ulcers - solcoseryl gel (or Actovegin), sea buckthorn or rosehip oil, oil solutions of vitamins A or E. If rashes appear on the lips or skin around the mouth, you can use Zovirax cream or acyclovir. In severe cases of the disease, it is necessary to use drugs against the herpes virus, but they must be prescribed by a doctor.
In general, it is dangerous to treat severe forms of stomatitis at home, especially such as Vincent’s ulcerative necrotizing stomatitis. To combat it, antibiotics will be required, which should be selected by the attending physician.