Publication date: March 13, 2022.
Information on this page was updated on December 31, 2021.
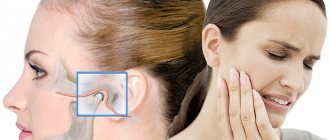
TMJ dysfunction is a fairly common pathology these days, as it is largely caused by stress factors. Here it can be difficult to understand what is primary and what is secondary, because people with joint dysfunction usually come with bite pathology, pathology of the musculoskeletal system (curvature of the spine, neck). Therefore, joint treatment is a complex story. It happens that the primary pathology is a pathology of the joint, and sometimes it is the musculoskeletal system.
Comprehensive treatment of TMJ
When the doctor has determined the cause of the joint pathology, or causes, he determines the patient's readiness for a comprehensive treatment plan. In addition to the orthodontist, an osteopath or chiropractor may be involved, or even an orthopedist if more complex correction of the musculoskeletal system is required.
The patient should be aware that it is possible to straighten the jaw using a splint or splint, but this will not solve the problem of malocclusion. Orthodontic treatment will be required to correct the bite. If you have already had orthodontic treatment before, then it is more difficult to decide on repeated treatment.
Therefore, first the problem with the joint is solved using a splint or joint splint, then bite correction is carried out, and, if necessary, prosthetics. In parallel, work is underway with an osteopath to restore the muscular corset of the back and neck.
It happens that a patient refuses treatment with braces after the problem with the joint has been resolved. In this case, we warn him about the need to wear a joint splint constantly in order to avoid the recurrence of old problems with the TMJ. After all, a relapse can happen quite quickly due to stress.
Diagnostics
When there is pain in the jaw, the patient first seeks advice from a dentist.
A dental examination includes the following steps.
- Clarifying patient complaints and collecting anamnesis. Since the main complaint is pain in the jaw, the time of its appearance (at night, during the day), the nature of the pain (sharp, dull, pulsating, aching), and duration (constant, paroxysmal) are specified.
- Examination of the oral cavity with assessment of the condition of the mucous membrane, tongue, gums, determination of the type of bite.
- Examination of the surfaces of all teeth using a probe and mirrors, identifying the integrity of the dentition, detecting defects in the hard tissues of the teeth.
- The percussion method is used to determine caries complications.
- Thermodiagnostics is used to identify pain reactions.
What may be the symptoms of TMJ dysfunction?
- Tenderness or pain in the area of one or both TMJs at rest or when opening the mouth.
- Crunching, clicking, crepitation and other noises in the area of one or both TMJs when opening the mouth.
- History of TMJ injuries (previous), incl. dislocation, subluxation, chronic subluxation.
- Restrictions in the mobility of the TMJ, restrictions in opening the mouth.
- Excessive tone of the masticatory muscles, bruxism (“grinding” of teeth in sleep, at rest).
- Asymmetry of the chin, lips, lip frenulum, asymmetry of mouth opening, S-shaped opening.
- Suspicion of a forced position of the lower jaw.
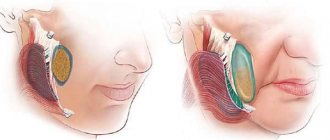
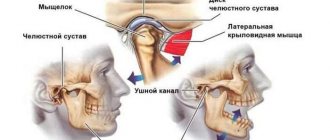
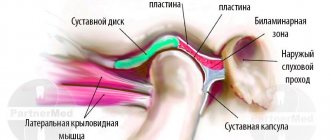
Structure of the TMJ
The presence of one or more of the above symptoms may indicate TMJ dysfunction.
Traditional orthodontic treatment does not address TMJ dysfunction. During orthodontic treatment, the severity of dysfunction may not change, decrease or increase. At the moment, in the world scientific orthodontic literature there is no convincing data on the connection between orthodontic treatment and the condition of TMJ. Deterioration of the joint after treatment may have nothing to do with this treatment.
Note! Even in the absence of visible clinical manifestations of joint dysfunction, hidden disorders may occur that require special diagnostics to identify them.
If there is a forced incorrect position of the lower jaw, its position may change during the treatment process with changes and complication of the treatment plan (the need to remove individual teeth, increasing the duration of treatment). A reliably forced position cannot be diagnosed by traditional orthodontic methods; to verify its presence, as a rule, a special analysis is required (manual functional analysis, determination of the central relationship of the jaws), the use of a special articular splint for a period of several months, which, however, does not give 100 % guarantees.
To conduct a detailed articular diagnosis, explain the specifics of your case, and further manufacture an articular splint, you can make an appointment with an orthodontist who deals with the issue of TMJ dysfunction.
TMJ dysfunction is a chronic condition that can be compensated, but not cured (i.e., it is possible to eliminate symptoms, however, pathological changes in the joints, if they have already occurred, will most likely persist).
Pediatric dentist
Treatment and extraction of teeth for patients under 18 years of age is carried out by a pediatric dentist. When working with young patients, the primary task is to find contact with the child and get him ready for treatment, because almost all children enter any medical office with fear. In addition, the children's doctor needs to tell the child's parents how to carry out home oral hygiene for the baby, what products to use, when the physiological change of teeth occurs, etc.
Maintaining dental health from a very early age is necessary for the normal formation of the dental system.
What happens if TMJ dysfunction is not treated?
If the dysfunction is not treated, the compensatory capabilities of the body may sooner or later be exhausted, the symptoms will worsen, the pathology will begin to progress, causing greater discomfort (sometimes for several years), thereby affecting the deterioration of the function of the dental system.
In order to try to prevent this and carry out treatment taking into account the individual characteristics of the structure and functioning of the temporomandibular joints, patients are usually offered the following approach.
Dental hygienist
A dental hygienist has a secondary professional medical education. A prerequisite for working as a hygienist is to successfully complete the course “Preventive Dentistry”. What does a dental hygienist do:
- professional oral hygiene;
- treatment of gums with the Vector device;
- whitening;
- provides training in proper oral hygiene;
- selection of personal hygiene products;
- deals with the prevention of gum disease in adults and children.
In short, the main area of work of a dental hygienist is the removal of dental plaque (tartar, plaque). It is important to see a hygienist every six months to maintain oral health.
Treatment method for TMJ dysfunction
1. Diagnosis of TMJ dysfunction.
- When diagnosing a joint in the clinic, a series of measurements and tests are carried out, all sensations in the joint area are recorded (discomfort, clicks, pain, deviation of the jaw when opening and closing), the difference in sensations in the right and left joint.
- The orthodontist also takes impressions of the jaws and takes photographs of the face and intraoral photographs, and also performs three-dimensional computed tomography of the face (3D CT); if necessary, the doctor can give a referral for an additional study - magnetic resonance imaging of the TMJ (MRI).
- Often, the orthodontist, in addition to manual functional analysis, conducts a visual assessment of: posture, symmetry of the shoulder girdle, shoulder blades, hip bone structures, etc., performs the necessary tests and photographs. Based on the results, it is possible to schedule a consultation with an osteopath or chiropractor to jointly manage the patient. Related specialists (orthopedist, surgeon, periodontist) can also be involved in drawing up a treatment plan.
What exercises are prescribed to patients to normalize the work and relax the masticatory muscles?
Exercise No. 1
Draw a vertical line on the mirror with a marker, stand opposite so that the line divides your face into the right and left halves, place your fingers on the area of the articular heads, lift your tongue up and back, open and close your mouth along the line (it may not work right away), 2-3 times /day 30 repetitions. There is no need to open your mouth wide (a comfortable width), the main thing is symmetrically (so that the jaw does not “move” in any direction). If there is a click, open until it clicks.
Exercise No. 2 (cycle)
Do it whenever possible, for example, in front of the TV, at the computer, or in a traffic jam while driving. Open and close your mouth without closing your teeth for 30 seconds, then alternately reach your right and left cheeks with your tongue for 30 seconds. Open - close your mouth again, then for 30 seconds move your tongue in a circle inside the vestibule (behind the lips), first in one direction, then in the other direction (clockwise - counterclockwise), open again - close your mouth, etc.. For this a half-hour cycle, the teeth should not touch, the lips should be closed. If you want to close your mouth or swallow, place your tongue between your teeth. Repeat the cycle for 20-30 minutes 2-3 times/day
Occlusive therapy for TMJ dysfunction
After diagnosis, the patient is scheduled for an appointment with the orthodontist to determine the central relationship of the jaws (“true” position of the lower jaw, the position in which your joint and chewing muscles will be most comfortable).
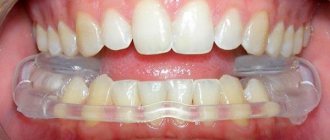
In order to more accurately establish and fix this position, an occlusal splint (splint) will be individually made for the patient from a special plastic, which is erased as it is worn. The splint must be worn constantly (sleeping, talking, eating in it if possible) - this is the meaning of occlusion therapy, which will help the joint and masticatory muscles rebuild into the most comfortable functional state.
Cleaning and caring for the splint is very simple - after eating (as well as while brushing your teeth), brush with a soft brush with toothpaste or soap.
Installation of a brace system for a patient with TMJ dysfunction
Installation of a brace system on the upper jaw is carried out on average after 3 months of occlusion therapy. The splint is adjusted once every 1-2 weeks, or at the discretion of the doctor, until the main complaints from the TMJ are eliminated (in parallel with the alignment of the teeth in the upper jaw), then a brace system is installed on the lower jaw with partial reduction (grinding) of the interfering parts of the occlusal tires, or complete removal. Here the patient needs to be patient - the process may take several months.
At the same time, the new position of the lower jaw is monitored: repeated manual functional analysis, photometry, bite registration is possible, computed tomography of the face during treatment, continuation of orthodontic treatment with a brace system.
Upon completion of orthodontic treatment, final monitoring of the position of the lower jaw follows (manual functional analysis, photometry, bite registration, 3D CT scan of the face upon completion (after) treatment).
Joint splint
Joint splint with braces
Causes of jaw pain not related to dental disorders
Neuralgia
When the trigeminal nerve, which is responsible for the sensitivity of the face and oral cavity, is damaged, the pain is strong, sharp, reminiscent of the pain of pulpitis. Often patients with trigeminal neuralgia undergo unnecessary dental treatment with depulpation or tooth extraction, but the pain syndrome persists.
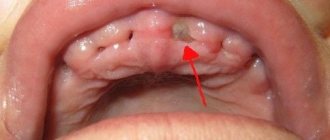
Sialolithiasis
Salivary stone disease is characterized by the formation of stones in the ducts of the large salivary glands. Since the salivary glands are located in the mouth, pain during their inflammation also affects other nearby organs of the oral cavity, in particular the jaw.
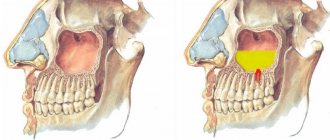
Sinusitis
When the mucous membrane of the maxillary cavity becomes inflamed, increasing swelling and accumulation of exudate cause pain spreading to the upper jaw area from the side of the affected sinus.
Otitis
Sometimes the symptoms of otitis media are similar to toothache. With inflammation of the middle ear, pain often radiates to the jaw. The pain is sharp, shooting, aggravated by chewing and swallowing.
Submandibular lymphadenopathy
Enlargement of the submandibular lymph nodes is observed in diseases of the tonsils, acute respiratory viral infections, stomatitis, and oncological tumors. Pain under the jaw is often accompanied by limited range of motion - it is difficult for the patient to bend and turn his head, or open his mouth wide.
Diseases of the cardiovascular system
Irradiation of pain into the lower jaw can be observed during an attack of angina and myocardial infarction. A characteristic symptom of coronary heart disease is burning, pressing pain behind the sternum. But with an atypical course of a heart attack, retrosternal pain may be completely absent, only reflected pain comes to the fore: in the left arm, in the neck, in the face, in the jaw.